Understanding Hysterectomy: Procedure and Health Conditions
If you’re considering a hysterectomy or have recently undergone the procedure, it’s important to understand the potential effects it may have on your health and well-being. A hysterectomy involves the removal of the uterus and can be performed for various health conditions. While it does not directly cause weight loss, some individuals may experience temporary weight loss due to post-surgery nausea or improvements in symptoms related to conditions like fibroids or endometriosis. On the other hand, weight gain can be a potential side effect, especially for premenopausal women who still have their ovaries. It’s crucial to discuss any unintended weight changes with your doctor, along with other potential side effects such as the cessation of menstruation, loss of fertility, and potential menopausal symptoms. While recovery from the procedure may require avoiding strenuous activity for a few weeks, low-impact exercises like yoga or swimming can typically be resumed within a few weeks as well.
Table of Contents
ToggleUnderstanding Hysterectomy: Procedure and Health Conditions
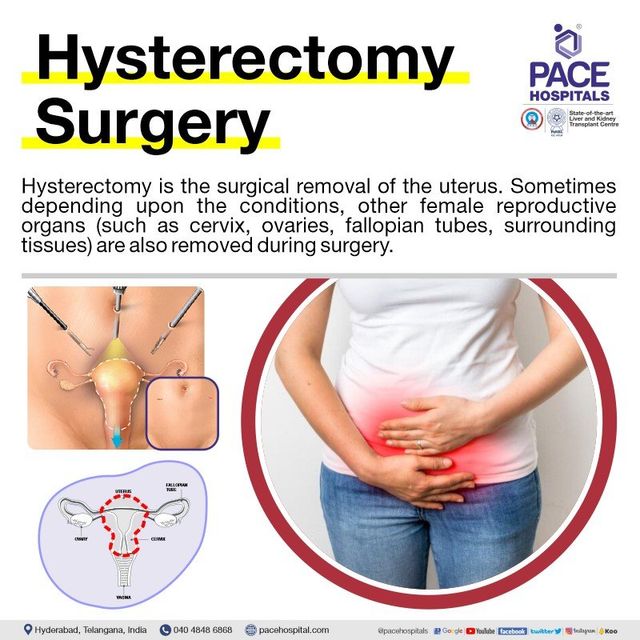
Hysterectomy is a surgical procedure that removes the uterus and can be done for various health conditions. It is a common procedure that is often performed to alleviate symptoms or treat certain medical conditions. Understanding what a hysterectomy entails and its potential effects on your health is important in making informed decisions about your healthcare.
What is a Hysterectomy?
A hysterectomy is a surgical procedure that involves the removal of the uterus. The uterus, also known as the womb, is the organ where a fertilized egg implants and develops during pregnancy. By removing the uterus, a hysterectomy permanently stops menstruation and prevents future pregnancies.
Common Reasons for Hysterectomy
There are several reasons why a hysterectomy may be recommended. Some of the most common reasons include:
-
Uterine Fibroids: Uterine fibroids are noncancerous growths that form in or around the uterus. They can cause symptoms such as heavy or prolonged menstrual bleeding, pelvic pain, and pressure.
-
Endometriosis: Endometriosis is a condition in which the tissue that normally lines the uterus grows outside the uterus. This can cause pelvic pain, abnormal bleeding, and fertility problems.
-
Adenomyosis: Adenomyosis is a condition in which the tissue that lines the uterus grows into the walls of the uterus. This can cause heavy bleeding, severe menstrual cramps, and an enlarged uterus.
-
Uterine Prolapse: Uterine prolapse occurs when the uterus descends into the vaginal canal due to weakened pelvic floor muscles. This can cause discomfort, urinary incontinence, and difficulty with bowel movements.
-
Abnormal Uterine Bleeding: Persistent or excessive uterine bleeding that does not respond to other treatments may warrant a hysterectomy.
-
Cancer: In some cases, a hysterectomy may be performed as part of the treatment for uterine, ovarian, or cervical cancer.
Types of Hysterectomy Procedures
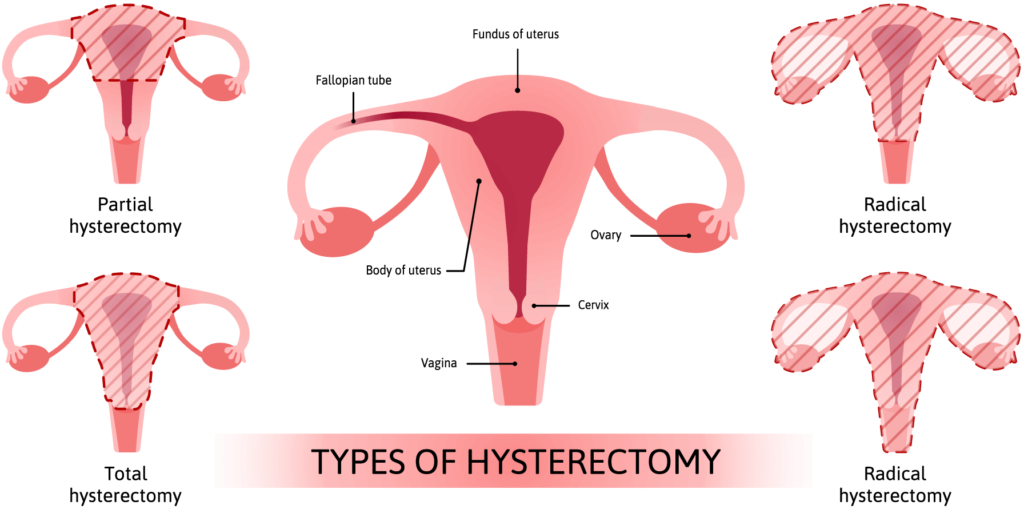
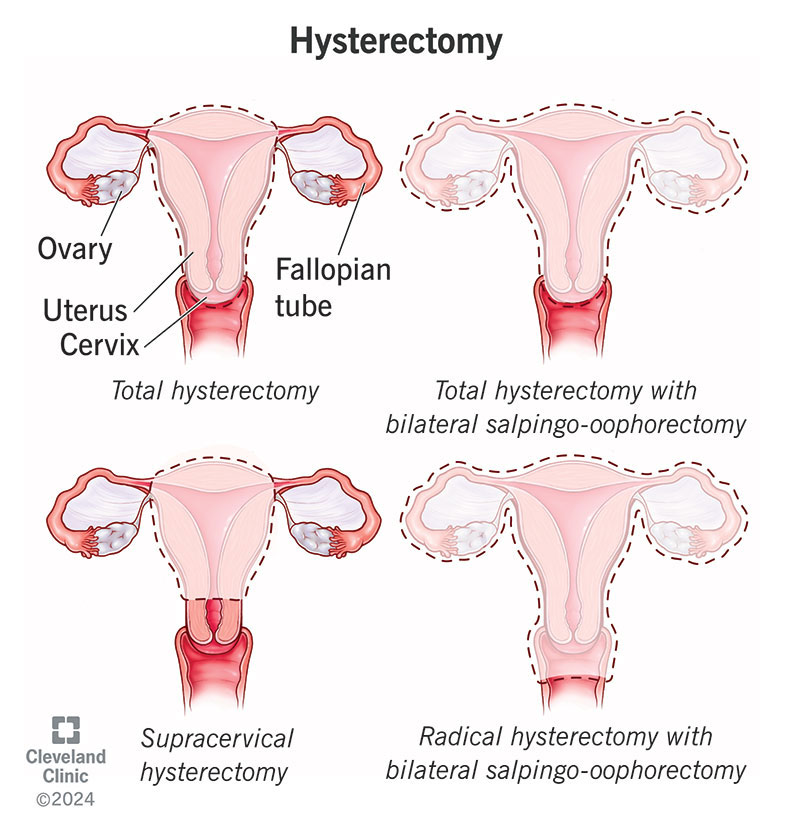
There are different types of hysterectomy procedures, depending on the extent of the surgery and the underlying condition. The most common types of hysterectomy include:
-
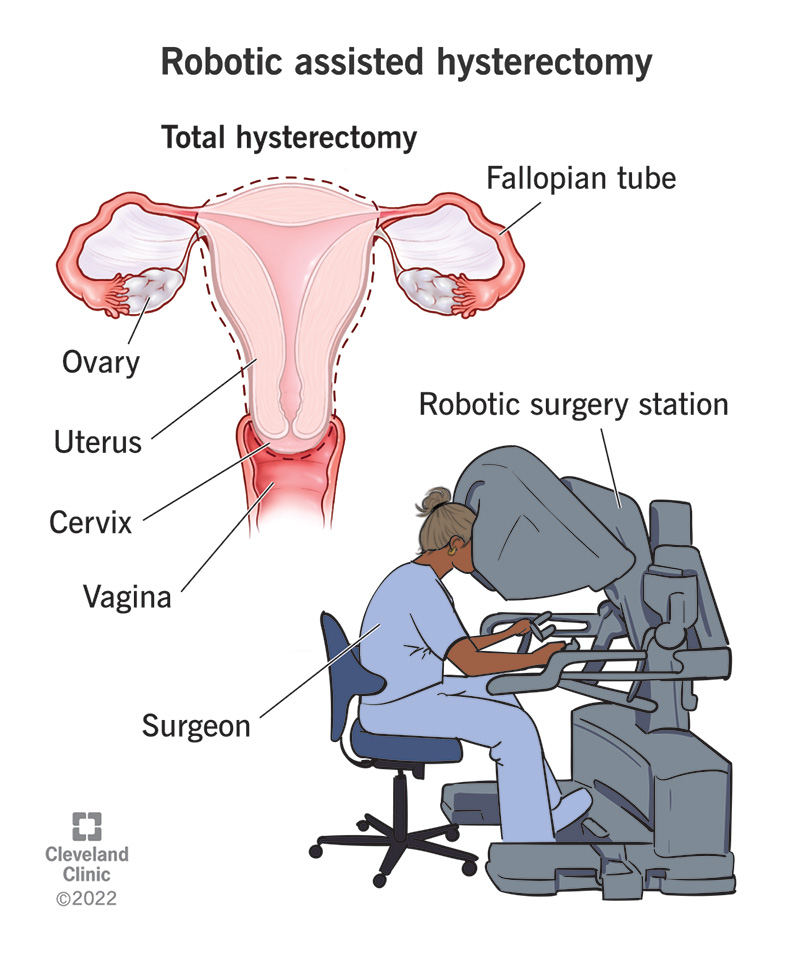
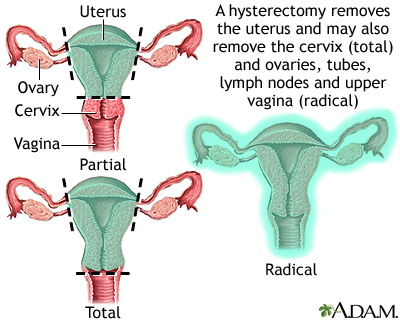
Total Hysterectomy: In a total hysterectomy, the entire uterus, including the cervix, is removed.
-
Partial Hysterectomy: A partial hysterectomy involves the removal of the upper part of the uterus, while leaving the cervix intact.
-
Radical Hysterectomy: A radical hysterectomy is performed for certain gynecologic cancers. It involves the removal of the uterus, cervix, the tissue surrounding the cervix, and possibly the upper part of the vagina.
-
Minimally Invasive Hysterectomy: Minimally invasive hysterectomy techniques, such as laparoscopic or robotic-assisted surgeries, involve smaller incisions and shorter recovery times compared to traditional open surgery.
Preparing for a Hysterectomy
Before undergoing a hysterectomy, it is essential to prepare both physically and emotionally for the procedure. Here are some guidelines to help you prepare:
-
Consultation with the Surgeon: Schedule a consultation with your surgeon to discuss your medical history, treatment options, and any concerns you may have.
-
Medical Evaluation: Your surgeon may order preoperative tests, such as blood work and imaging studies, to evaluate your overall health and identify any potential risks or complications.
-
Preoperative Instructions: Follow any preoperative instructions provided by your surgeon, such as fasting guidelines or medication restrictions.
-
Mental and Emotional Preparation: As a major surgery, a hysterectomy can have emotional implications. It is important to address any fears or concerns you may have and seek support from loved ones or support groups, if needed.
-
Clearing the Bowels and Bladder: Your surgeon may instruct you to empty your bowels and bladder before the surgery to reduce the risk of complications during the procedure.
The Hysterectomy Procedure
During a hysterectomy, several key steps are involved. Understanding the procedure can help alleviate any anxieties you may have. The general steps of a hysterectomy include:
-
Anesthesia: Before the surgery begins, you will be given anesthesia to ensure that you are comfortable and pain-free during the procedure. The type of anesthesia used can vary depending on the surgical approach and individual patient needs.
-
Surgical Techniques: The surgeon will choose the most appropriate surgical technique based on the specific condition being treated and other factors such as the patient’s medical history and the surgeon’s expertise.
-
Removal of the Uterus: The uterus is carefully removed, either in its entirety in a total hysterectomy or in part in a partial hysterectomy. The surgeon will take steps to minimize bleeding and ensure the safety of surrounding organs and structures.
-
Potential Additional Procedures: In some cases, additional procedures may be performed during a hysterectomy. This could include the removal of the ovaries and fallopian tubes (oophorectomy and salpingectomy), removal of lymph nodes for cancer staging, or repair of pelvic floor support structures.
-
Length of the Procedure: The length of the hysterectomy procedure can vary depending on the complexity of the surgery and the chosen surgical approach. On average, a hysterectomy can take anywhere from one to three hours.
Recovery and Aftercare
After a hysterectomy, proper recovery and aftercare are crucial for healing and minimizing complications. Here are some important considerations:
-
Hospital Stay: The length of your hospital stay will depend on the type of hysterectomy performed and individual factors. In some cases, a hysterectomy can be performed as an outpatient procedure, meaning you can return home on the same day. However, more extensive surgeries may require a longer hospital stay.
-
Immediate Recovery: You can expect to experience some pain and discomfort in the days following your surgery. Pain management techniques, such as medication prescribed by your doctor, can help alleviate any discomfort.
-
Pain Management: Your surgeon will provide instructions for managing pain during your recovery, including prescribed pain medication and other techniques such as heat application or relaxation exercises.
-
Physical Activity Restrictions: For proper healing, it is essential to avoid strenuous activities, heavy lifting, and certain exercises for a few weeks after the surgery. However, low-impact activities like walking, yoga, or swimming are usually encouraged to promote circulation and reduce the risk of blood clots.
-
Resuming Daily Activities: Gradually reintroduce daily activities and self-care tasks such as showering, dressing, and light household chores. It is important to listen to your body and not push yourself too hard during this time.
-
Returning to Work: The time it takes to return to work will vary depending on the type of hysterectomy performed and the nature of your job. Desk jobs may allow for a quicker return, while physically demanding jobs may require additional time off.
-
Follow-up Appointments: Regular follow-up appointments with your surgeon are essential to monitor your healing progress, address any concerns, and ensure a smooth recovery. Be sure to attend these appointments as scheduled.
Potential Side Effects of Hysterectomy
Hysterectomy can have several potential side effects, which may vary from person to person. Some common side effects include:
-
Cessation of Menstruation: Following a hysterectomy, menstruation will cease permanently since the uterus has been removed. This can be a relief for those who have experienced heavy or painful periods.
-
Loss of Fertility: Hysterectomy results in the inability to conceive and carry a pregnancy. If maintaining fertility is important to you, it is essential to discuss this with your doctor before the surgery.
-
Menopausal Symptoms: Hysterectomy can induce menopause, especially if the ovaries are also removed during the procedure. This can lead to symptoms such as hot flashes, night sweats, mood swings, and vaginal dryness.
-
Psychological Impact: Some individuals may experience emotional and psychological changes following a hysterectomy. These can include feelings of loss, grief, or changes in body image. Openly discussing these concerns with a healthcare professional or seeking support from loved ones can be beneficial.
-
Urinary and Bowel Changes: Hysterectomy can sometimes cause changes in urinary and bowel function. These changes may include increased frequency of urination, urinary incontinence, or constipation. These symptoms are usually temporary but can be managed through lifestyle modifications and, if needed, additional treatment.
-
Sexual Function Changes: Hysterectomy may impact sexual function, including changes in libido or vaginal dryness. Open communication with your partner and healthcare provider can help address any concerns and explore potential solutions.
-
Hormonal Changes: If the ovaries are removed during a hysterectomy, hormone replacement therapy (HRT) may be necessary to manage the hormonal effects of menopause. Your doctor can discuss the potential benefits and risks of HRT and help determine if it is the right option for you.
Weight Loss After Hysterectomy
While a hysterectomy does not directly cause weight loss, some individuals may experience temporary weight loss following the procedure. This can be due to factors such as post-surgery nausea, decreased appetite, or improved symptoms of conditions such as fibroids or endometriosis. However, it is essential to note that weight loss should not be the primary focus after a hysterectomy. Instead, emphasis should be placed on overall health and well-being.
Factors Affecting Weight Loss
Various factors can influence weight loss after a hysterectomy. These can include individual metabolism, hormone levels, nutritional intake, and physical activity levels. It is important to maintain a balanced and nutritious diet while listening to your body’s hunger and fullness cues.
Temporary Weight Loss
Temporary weight loss following a hysterectomy may occur due to factors such as decreased appetite or water loss. However, it is not uncommon for weight to stabilize or return to pre-surgery levels over time.
Maintaining a Healthy Weight
Maintaining a healthy weight after a hysterectomy involves maintaining a balanced lifestyle. This includes eating a well-rounded diet, engaging in regular physical activity, managing stress levels, and getting adequate sleep. It is important to focus on overall health rather than becoming fixated on weight.
Other Considerations
There are a few additional considerations to keep in mind when it comes to hysterectomy:
-
Discussion with the Doctor: It is crucial to have open and honest communication with your healthcare provider throughout the entire process. This includes discussing any concerns, potential risks, and expected outcomes of the surgery.
-
Intended and Unintended Weight Changes: It is important to differentiate between intended weight changes, such as weight loss due to a healthier lifestyle, and unintended weight changes that may require medical attention. Discuss any significant weight changes with your doctor to rule out any underlying issues.
-
Importance of Monitoring Weight: Regularly monitoring your weight can help you stay aware of any significant changes and seek medical guidance if necessary. However, it is important not to obsess over the numbers on the scale and focus on overall well-being.
-
Healthy Lifestyle and Support: Adopting and maintaining a healthy lifestyle can positively impact your overall health and well-being. Seek support from loved ones, healthcare professionals, or support groups to help you navigate the physical and emotional aspects of a hysterectomy.
In conclusion, understanding the procedure and potential effects of a hysterectomy is essential for making informed decisions about your health. While a hysterectomy can provide relief for certain health conditions, it is important to discuss your concerns, expectations, and potential side effects with your healthcare provider. By taking the time to prepare, following proper aftercare guidelines, and maintaining a healthy lifestyle, you can optimize your recovery and overall well-being after a hysterectomy.
Understanding Hysterectomy: Learn about the procedure, health conditions it treats, and potential effects on weight and well-being. Make informed decisions about your healthcare.